- Overview: What Are the Early Signs of Squamous Cell Carcinoma?
- Most Common Early Symptoms
- How Early Symptoms Usually Develop
- Less Common or Subtle Symptoms
- Symptoms Suggesting Progression
- Appearance in Different Skin Tones
- Why Symptoms Form – Biological Explanation
- How Doctors Diagnose Squamous Cell Carcinoma
- Risk Factors That Increase Likelihood
- When to See a Doctor
- Self-Monitoring – What to Track Monthly
- Prevention & Skin Protection Habits
- Lifestyle & Skin Care Tips for Those Monitoring Lesions
- Emotional Wellness & Coping
- Myths vs Facts
- Frequently Asked Questions (FAQ)
- Internal Links – Continue Learning
- References
Squamous cell carcinoma (SCC) is the second most common type of skin cancer, developing from squamous cells located in the outer layers of the skin. It often begins as rough patches, scaly growths, or non-healing sores that may appear harmless at first. Because symptoms may resemble rashes, eczema, or sun-damaged skin, early stages are commonly overlooked. Understanding early warning signs can support timely evaluation and help prevent deeper tissue involvement (National Cancer Institute).
SCC most frequently forms on areas exposed to ultraviolet (UV) radiation – such as the face, ears, scalp, lips, neck, and hands – but it can develop anywhere, including inside the mouth or under nails in rare cases. While many cases progress slowly, some forms of SCC may grow more aggressively than basal cell carcinoma, making early recognition especially important (Mayo Clinic).
Overview: What Are the Early Signs of Squamous Cell Carcinoma?
Early SCC usually begins as persistent skin changes. A patch may look dry, crusted, or wart-like. Some individuals notice a firm red nodule, while others develop a flat sore that repeatedly heals and reopens. The key indicator is persistence – normal skin injuries typically heal within weeks, but SCC-related lesions remain or worsen over time (American Cancer Society).
Unlike melanoma, which often grows from moles, SCC typically starts on regular skin surfaces. It can begin small, then gradually increase in thickness, scale, or discomfort. Early medical consultation is encouraged for any spot that bleeds, crusts, or does not heal.
Most Common Early Symptoms
Signs of SCC vary depending on location, skin type, and depth of growth. Early symptoms often include:
- Rough or scaly patch of skin that does not improve with moisturizers (Mayo Clinic)
- Persistent sore that bleeds, crusts, or reopens repeatedly
- Firm red bump or nodule that gradually enlarges
- Raised growth with a central depression or crust
- Wart-like growth that becomes tender or hard
- Crusty, scab-like lesion lasting over 4—6 weeks
- Thickened or rough skin patch in sun-exposed areas
Early SCC lesions may be mistaken for insect bites, scrapes, fungal patches, or keratosis. However, unlike temporary irritations, SCC lesions do not fully heal. A key warning sign is recurrence – if a sore improves slightly then returns, it may signal abnormal cell growth (NCI).
How Early Symptoms Usually Develop
Symptoms may begin subtly, often with dry or flaky skin. Over weeks or months, the area may thicken, crack, or bleed. Pain is not always present early – some early SCC patches feel rough to touch but remain painless. Others may itch or become sensitive when rubbed by clothing. Monitoring changes helps recognize patterns early.
- Week 1—4: Dry patch or small rough area appears
- 1—3 months: Area grows thicker or begins crusting
- Later: Nodule forms, bleeding increases, ulceration possible
SCC tends to grow outward and upward at first but can later spread downward into deeper layers, including nerves or bone if untreated. Early recognition improves treatment options significantly.
Less Common or Subtle Symptoms
Not all squamous cell carcinoma begins with dramatic or obvious skin changes. In some cases, early signs appear as mild irritation or small patches that look like common skin problems. Many individuals confuse early SCC with eczema, psoriasis, or chapped skin. Because symptoms develop gradually, subtle changes may last for weeks or even months before being noticed (Mayo Clinic).
Subtle early symptoms may include:
- Dry, scaly patch that flakes but returns after peeling
- Red or brown crusty spot that never fully heals
- Slight thickening of skin compared to surrounding areas
- Flat patch with rough texture like sandpaper to touch
- Hard or keratinized bump resembling a wart
- New skin growth that slowly increases in diameter
- Itching or burning sensation without rash-related triggers
Sometimes SCC begins as actinic keratosis – a precancerous lesion caused by long-term sun exposure. Actinic keratosis may appear as rough, gritty patches on the face, scalp, ears, or hands. Not all AKs become cancer, but some may progress into SCC over time (National Cancer Institute).
Symptoms Suggesting Progression
If early warning signs are missed or the lesion continues to grow, SCC may progress and become more noticeable. Progression does not always mean severe disease – rather, it means the growth is expanding and may involve deeper tissues. While many SCC lesions are detected early, untreated cases may lead to more advanced symptoms (American Cancer Society).
Signs of progression or deeper invasion may include:
- Persistent bleeding from minor friction or touch
- Raised edges with a central depression or sore
- Ulceration forming an open wound-like center
- Crust or scab that reforms repeatedly
- Firm, tender growth or wart-like surface
- Pain or increased sensitivity over time
- Spread to nearby lymph nodes in advanced cases (swelling beneath jaw or groin)
A rolled or elevated border with crusted center is one of the hallmark progressive SCC signs. In later stages, lesions may produce a foul odor or discharge if infection occurs. Pain and swelling may appear once nerves or deeper areas are affected. While most SCC does not metastasize quickly, the possibility increases if left untreated for long periods (WHO).
Appearance in Different Skin Tones
Symptoms can vary by skin type and pigmentation. On fair skin, SCC often appears pink, red, or flesh-colored. On darker skin tones, lesions may appear brown, gray, or darker than surrounding skin. Recognizing variation is important for equitable awareness.
- Light skin: pink or red patch, scaly texture, visible crusting
- Medium skin: tan or reddish-brown rough spot
- Dark skin: darkened or blackish patch that thickens gradually
SCC on lips may appear as a scaly rough patch or persistent chapped area. On nails, it may present as dark streaks, nail lifting, or persistent swelling. These are uncommon, but possible presentations worth monitoring (Mayo Clinic).
Why Symptoms Form – Biological Explanation
Squamous cell carcinoma begins when UV radiation (sun or tanning beds) damages DNA in skin cells. Instead of repairing themselves, the cells begin multiplying uncontrollably. As abnormal cells accumulate, surface texture changes – becoming rough, crusted, or raised. When growth pushes upward, raised nodules form; when growth spreads downward, ulceration or tenderness may appear (NCI).
How cellular changes become visible symptoms:
- Excess keratin buildup → scaly or rough texture
- Abnormal blood supply → red, inflamed appearance
- Cell overgrowth → bumps or nodules form
- Tissue breakdown → sores or ulceration
Persistent DNA damage from sun exposure explains why outdoor workers, athletes, and people living in sunny climates have higher rates of SCC. Early UV protection and routine skin checks may reduce risk significantly.
How Doctors Diagnose Squamous Cell Carcinoma
Because SCC commonly begins on the skin surface, diagnosis often starts with a visual examination by a dermatologist or healthcare provider. They may assess how long the lesion has been present, whether it bleeds, its texture, and how it responds to normal healing. If cancer is suspected, a biopsy is typically performed to confirm the presence of cancer cells (National Cancer Institute).
Common diagnostic methods include:
- Clinical examination: Assessment of color, surface, scaling, and lesion shape.
- Dermoscopy: Close-up magnified evaluation of blood vessels, scales, and pigmentation.
- Skin biopsy: Small tissue sample removed and examined under microscope.
- Shave biopsy: Surface tissue sample removed for testing.
- Punch biopsy: Circular tool collects deeper tissue sample.
In cases where SCC is large, recurring, or suspected of reaching deeper tissues, additional scans like CT, ultrasound, or MRI may be used to evaluate spread to cartilage, bone, or lymph nodes (Mayo Clinic).
Risk Factors That Increase Likelihood
Anyone can develop squamous cell carcinoma, but certain factors raise risk. Most are related to UV exposure, but immune health, genetics, and lifestyle also contribute. A person may have multiple risk factors and never develop SCC – or have none and still experience it (American Cancer Society).
Key risk factors include:
- Frequent or intense sun exposure over many years
- History of sunburns – especially blistering burns in youth
- Indoor tanning bed use
- Fair skin, freckles, red/blonde hair
- Age above 50, though younger adults can develop SCC
- Previous skin cancers or actinic keratoses
- Weakened immune system (transplant recipients, HIV, immune disorders)
- Long-term exposure to chemicals such as arsenic
- Smoking, especially for SCC on the lips or mouth
- HPV infection in certain skin or mucosal areas
Outdoor workers such as construction laborers, farmers, lifeguards, and athletes may have higher lifetime UV exposure. Sunscreen and protective clothing are especially helpful for these groups. People with dark skin tones have lower overall incidence, but when SCC develops, it may appear in less-exposed areas like legs, feet, or under nails.
When to See a Doctor
It is recommended to seek medical evaluation if:
- A sore or patch does not heal within 4—6 weeks
- Lesion keeps scabbing or reopening after healing attempts
- Growth changes size, shape, texture or becomes thicker
- Spot bleeds with minimal contact
- Nodule becomes painful, itchy, or tender
- Edges appear raised or rolled
Delaying evaluation allows the lesion to expand and may require more complex treatment later. Early diagnosis often leads to minimally invasive care (WHO).
Self-Monitoring – What to Track Monthly
Routine skin self-checks allow individuals to detect small changes before they progress. Using a mirror or smartphone camera may help track subtle developments. Checking once per month is a useful habit, especially after sun-exposure seasons.
- Take photos to compare size & texture month-to-month.
- Note if color darkens, reddens, or becomes shiny.
- Observe if growth becomes raised or more firm.
- Watch for flaky or crusting behavior after peeling.
- Track bleeding frequency when rubbed or washed.
If changes are noticeable over time, or symptoms persist, evaluation is recommended. Even non-cancerous actinic keratoses benefit from monitoring because some may progress into SCC.
Prevention & Skin Protection Habits
While prevention is never absolute, sun-safety practices help reduce risk significantly. UV exposure is the most preventable contributing factor. Protective strategies are beneficial for all skin types (NCI).
Helpful prevention habits:
- Use SPF 30+ sunscreen daily on exposed skin.
- Reapply sunscreen every 2 hours, especially when sweating or swimming.
- Wear protective clothing – hats, sunglasses, long sleeves.
- Seek shade when UV rays are strongest (10am—4pm).
- Avoid tanning beds – concentrated artificial UV causes DNA damage.
- Perform monthly skin checks to detect new lesions.
After outdoor activity, examine sun-exposed areas more closely. This includes the face, neck, arms, chest, shoulders, hands, and scalp – especially for men with thinning hair.
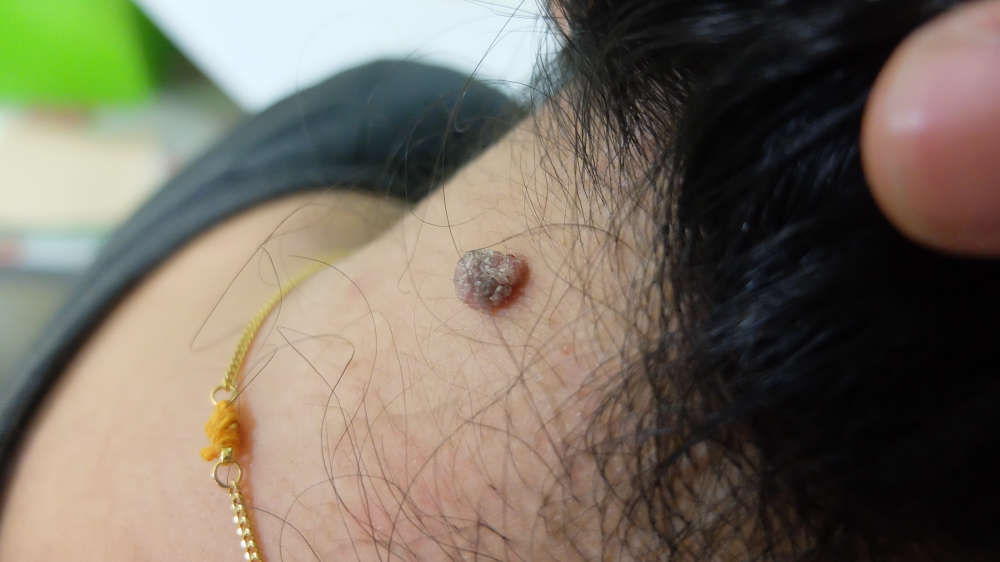
Lifestyle & Skin Care Tips for Those Monitoring Lesions
While lifestyle changes do not heal squamous cell carcinoma, they may support comfort and reduce irritation during monitoring or evaluation. Gentle care helps protect the skin and may prevent further trauma to suspicious areas. These habits maintain skin health while providing peace of mind during observation (National Cancer Institute).
- Keep skin clean and moisturized using fragrance-free products.
- Use SPF 30+ sunscreen on exposed skin daily.
- Wear protective clothing (wide-brim hat, long sleeves) outdoors.
- Avoid scratching, picking, or peeling crusting lesions.
- Reduce friction from tight clothing over affected areas.
- Apply gentle cool compresses for irritation relief.
- Monitor for bleeding or growth changes and record dates.
Healthy diet and hydration contribute to general well-being. Foods rich in antioxidants may help support skin health – such as blueberries, leafy greens, nuts, olive oil, and fish. While nutrition does not treat SCC, it may benefit overall skin resilience and recovery after medical procedures.
Emotional Wellness & Coping
Finding a new skin lesion or dealing with repeated bleeding can lead to worry or uncertainty. Many people hesitate to seek evaluation, hoping the lesion will heal with time. Understanding warning signs and knowing when to ask for help can reduce stress. Discussing concerns with someone trusted may also provide comfort (WHO).
Helpful emotional coping ideas:
- Talk with family or friends to ease worry.
- Keep notes and photos – documentation builds confidence and clarity.
- Practice calming routines, deep breathing, and short mindful breaks.
- Create self-care moments like warm showers, reading, or outdoor walks.
Many individuals feel more empowered once they understand that SCC is often highly treatable when found early. Awareness encourages timely decisions rather than fear-based waiting.
Myths vs Facts
Misinformation sometimes leads people to ignore early lesions. Separating fact from myth encourages faster evaluation.
- Myth: If it doesn’t hurt, it’s not cancer.
Fact: Early SCC is often painless and only becomes tender later. - Myth: Only older adults get SCC.
Fact: More common with age, but younger people with UV exposure may also develop it. - Myth: A lesion must grow quickly to be dangerous.
Fact: SCC may grow slowly but still cause deep skin damage over time. - Myth: Sunscreen is only needed in summer.
Fact: UV rays affect skin year-round, even on cloudy days. - Myth: If it scabs over once, it’s healed.
Fact: Recurrent scabbing is one of the strongest early warning signs.
Frequently Asked Questions (FAQ)
Q: Can squamous cell carcinoma appear unexpectedly?
A: Yes. Some lesions develop gradually, while others seem to appear suddenly but were previously unnoticed (Mayo Clinic).
Q: Does SCC always bleed?
A: No. Many early lesions do not bleed. Bleeding often appears in later stages or with friction.
Q: Does SCC only grow where sunlight reaches?
A: Mostly yes – but it can appear anywhere, including the mouth, genitals, and under nails.
Q: What color can SCC be?
A: Red, pink, brown, skin-colored, or darker depending on skin tone.
Q: How long can SCC stay unnoticed?
A: Months or years – growth is often slow, which is why monitoring matters.
Q: Should I wait to see if a sore heals?
A: If healing does not occur within 4—6 weeks or it repeatedly returns, evaluation is recommended.
Q: Can SCC spread?
A: Yes, though not always quickly. Advanced cases may spread deeper or to lymph nodes without treatment (American Cancer Society).
Internal Links – Continue Learning
You may also find these helpful:
References
- National Cancer Institute — Squamous Cell Carcinoma
- Mayo Clinic — SCC Overview
- American Cancer Society — SCC Guide
- World Health Organization — Cancer Facts
Disclaimer: This information is for educational purposes only and is not medical advice. Talk to a healthcare provider about questions related to your health.