- Types of Breast Cancer Screening Tests
- Understanding Mammogram Results
- Who Should Get Breast Cancer Screening
- Preparing for Breast Cancer Screening
- Benefits and Limitations of Screening
- Making Screening Decisions
- Common Myths and Misunderstandings
- Myth: Mammograms Cause Cancer
- Myth: Finding a Lump Always Means Cancer
- Myth: Young Women Don't Need to Think About Breast Cancer
- Key Takeaways
- Learn More
Breast cancer screening uses medical tests to check for cancer before symptoms appear. These tests help doctors find breast cancer early, when treatment works best. Understanding different screening methods helps you make informed decisions with your healthcare team.
Breast cancer screening includes several types of tests and exams. Each method has specific benefits and limitations. Learning about these options helps you know what to expect during screening appointments.
Types of Breast Cancer Screening Tests
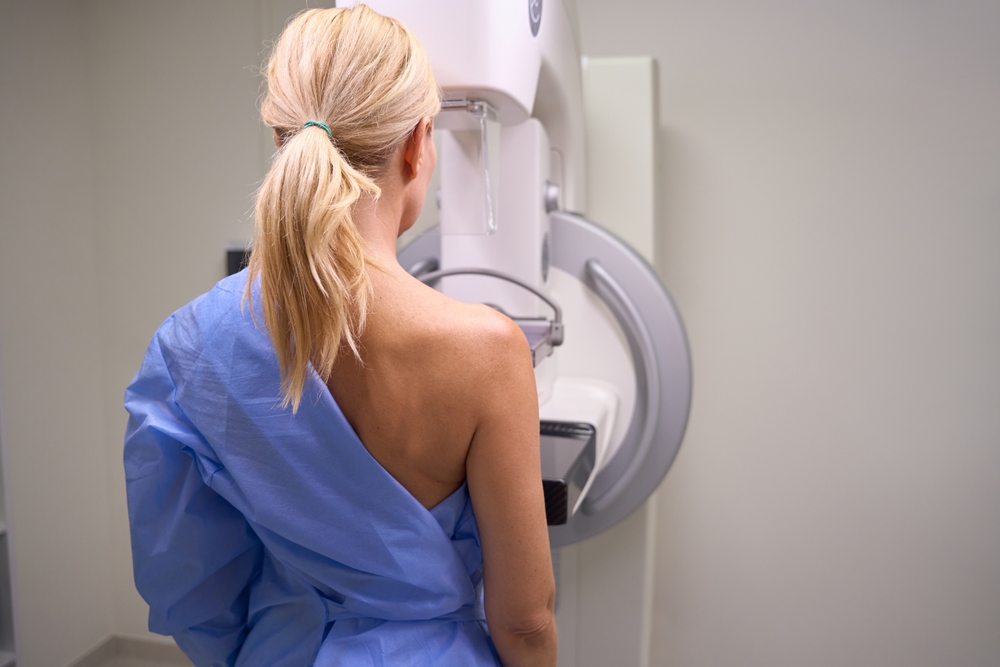
Mammography is the most common breast cancer screening test. This X-ray exam takes pictures of breast tissue to look for changes or growths. Digital mammograms use computer technology to create detailed images that doctors can examine closely.
Clinical breast exams involve a healthcare provider checking your breasts for lumps or changes. During this exam, the provider feels the breast tissue and nearby areas like the underarms and collarbone. This hands-on check can find changes that might not show up on imaging tests.
Breast self-exams help you learn how your breasts normally look and feel. Regular self-exams help you notice any changes between medical appointments. While self-exams are not formal screening tests, they help you stay aware of your breast health.
Additional imaging tests like breast ultrasound or MRI may be recommended for some people. These tests provide different types of images that can give doctors more information about breast tissue. Research shows these additional tests are most helpful for people with higher cancer risk.
Understanding Mammogram Results
Mammogram results use a scoring system called BI-RADS to describe findings. BI-RADS scores range from 0 to 6, with each number meaning something different. A score of 1 or 2 means normal or benign findings that do not require immediate action.
A BI-RADS score of 3 means probably benign findings that need follow-up imaging in six months. Scores of 4 or 5 suggest suspicious areas that need further testing like a biopsy. A score of 6 means known cancer that is being monitored during treatment.
Sometimes mammograms show dense breast tissue, which appears white on the images. Dense tissue can make it harder to see potential problems on mammograms. Studies suggest that knowing about breast density helps people and their doctors make better screening decisions.
False positive results happen when screening tests suggest cancer might be present, but further testing shows no cancer. According to the National Cancer Institute, false positives are common and affect about 1 in 10 women who get regular mammograms.
Who Should Get Breast Cancer Screening
Age is one factor that affects screening recommendations. Most medical organizations suggest that women of average risk begin regular mammograms between ages 40 and 50. The exact starting age depends on individual risk factors and preferences discussed with healthcare providers.
Family history of breast or ovarian cancer may mean starting screening earlier or getting additional tests. People with close relatives who had these cancers often have higher risk themselves. Genetic counseling can help determine if genetic testing might be helpful.
Previous breast problems like atypical cells or lobular carcinoma in situ may increase cancer risk. People with these conditions often need more frequent screening or additional types of tests. Healthcare providers create personalized screening plans based on individual medical history.
Certain genetic mutations like BRCA1 or BRCA2 significantly increase breast cancer risk. The U.S. Preventive Services Task Force recommends that people with these mutations follow special screening guidelines that often include MRI in addition to mammograms.
Preparing for Breast Cancer Screening
Timing your mammogram can affect comfort and image quality. Scheduling the exam for the week after your menstrual period often reduces breast tenderness. Breasts are typically less sensitive during this time, making the compression more comfortable.
Avoid using deodorant, powder, or lotion on your chest and underarms on the day of your mammogram. These products can show up as spots on the X-ray images, which might interfere with reading the results. Wearing a two-piece outfit makes it easier to undress for the exam.
Bring a list of any breast symptoms or concerns to discuss with the technologist or radiologist. Include information about previous breast problems, surgeries, or family history of breast cancer. This background information helps medical professionals interpret your results.
Know your insurance coverage for screening tests before your appointment. Most insurance plans cover recommended screening mammograms completely. Understanding your benefits helps you avoid unexpected costs and plan for regular screening.
Benefits and Limitations of Screening
Early detection through screening saves lives by finding cancer when it is most treatable. Research from the Centers for Disease Control and Prevention shows that mammography screening reduces breast cancer deaths by finding cancers before they can be felt.
Regular screening helps track changes in breast tissue over time. Having baseline images allows radiologists to compare new mammograms with previous ones. This comparison makes it easier to spot new or changing areas that need attention.
Screening has limitations and cannot find all cancers. Some cancers grow quickly between screening appointments, and others may not show up clearly on mammograms. Dense breast tissue can hide some cancers, making them harder to detect on standard mammograms.
Overdiagnosis is a concern with all cancer screening, including breast cancer screening. This means finding and treating cancers that might never have caused health problems. Experts continue studying ways to reduce overdiagnosis while maintaining the benefits of early detection.
Making Screening Decisions
Discussing screening with your healthcare provider helps create a plan that fits your individual situation. Consider your personal risk factors, preferences, and health goals when making screening decisions. Understanding what cancer screening involves helps prepare you for these important conversations.
Some people choose to start screening earlier or get additional tests based on their risk factors. Others may decide to delay screening or choose less frequent testing. There is no single right answer for everyone, and decisions can change over time as circumstances change.
Keep records of your screening tests and results. This information helps you and future healthcare providers understand your screening history. Having organized records makes it easier to ensure you stay up to date with recommended screening.
Stay informed about new research and screening recommendations. Medical guidelines sometimes change as researchers learn more about effective screening methods. Regular check-ups with your healthcare provider help you stay current with the latest recommendations.
Common Myths and Misunderstandings
Myth: Mammograms Cause Cancer
Some people worry that the radiation from mammograms increases cancer risk. The National Cancer Institute explains that modern mammography uses very low doses of radiation. The small radiation exposure is far outweighed by the benefits of early cancer detection.
Myth: Finding a Lump Always Means Cancer
Many breast lumps are not cancer. Studies show that about 80% of breast lumps are benign, meaning they are not cancerous. However, any new lump or change should be evaluated by a healthcare provider to determine the cause and appropriate follow-up.
Myth: Young Women Don’t Need to Think About Breast Cancer
While breast cancer is more common in older women, it can occur at any age. Young women should be aware of their breast health and report any changes to their healthcare providers. Knowing your family history and risk factors helps guide appropriate screening decisions at any age.
Key Takeaways
- Breast cancer screening uses tests like mammograms and clinical exams to find cancer before symptoms appear
- Mammography is the most widely used screening test, with results reported using the BI-RADS scoring system
- Screening recommendations depend on age, family history, genetic factors, and personal risk assessment
- Proper preparation includes scheduling at the right time and avoiding certain products on exam day
- Screening has both benefits and limitations, including the possibility of false positives and overdiagnosis
- Working with your healthcare provider helps create a personalized screening plan that fits your individual needs
Learn More
- National Cancer Institute Mammograms Fact Sheet – comprehensive information about mammography screening
- CDC Breast Cancer Screening Guidelines – current recommendations and research on screening benefits
- U.S. Preventive Services Task Force Recommendations – evidence-based screening guidelines for healthcare providers
- World Health Organization Breast Cancer Facts – global perspective on breast cancer prevention and screening
- Why Early Detection Matters – understanding the importance of finding cancer early
- How to Prepare for Cancer Screening – practical tips for getting ready for screening appointments
- ClinicalTrials.gov Breast Cancer Screening Studies – current research on new screening methods and technologies
Disclaimer: This information is for educational purposes only and is not medical advice. Talk to a healthcare provider about questions related to your health.