- Who Should Consider Lung Cancer Screening
- How Low-Dose CT Screening Works
- Benefits and Limitations of Screening
- What to Expect During and After Screening
- Making Decisions About Screening
- Beyond Screening: Reducing Lung Cancer Risk
- Common Myths and Misunderstandings
- Myth: Everyone Over 50 Should Get Lung Cancer Screening
- Myth: A Normal Screening Result Means You Will Never Get Lung Cancer
- Myth: Lung Cancer Screening Uses Dangerous Amounts of Radiation
- Key Takeaways
- Learn More
Lung cancer screening is a medical test that looks for lung cancer in people who have no symptoms. The main screening method uses low-dose computed tomography (LDCT) scans to create detailed pictures of the lungs. This screening can find lung cancer early, when treatment works best.
Not everyone needs lung cancer screening. Medical experts have specific guidelines about who should get screened. Understanding cancer screening basics helps people make informed decisions with their healthcare providers about whether screening is right for them.
Who Should Consider Lung Cancer Screening
The U.S. Preventive Services Task Force recommends lung cancer screening for people who meet specific criteria. These guidelines help identify those at highest risk who would benefit most from screening.
Current screening recommendations include adults aged 50 to 80 years who have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years. A pack-year means smoking one pack of cigarettes per day for one year. Someone who smoked two packs daily for 10 years also has a 20 pack-year history.
People should be in good health and able to have lung surgery if cancer is found. Those with serious health conditions that would prevent cancer treatment may not benefit from screening. Healthcare providers help determine if screening fits individual health situations.
How Low-Dose CT Screening Works
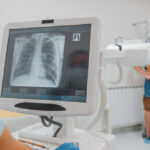
Low-dose computed tomography uses less radiation than regular CT scans while still creating clear images of the lungs. During the scan, patients lie on a table that slides through a large, donut-shaped machine. The process takes only a few minutes and causes no pain.
The CT scanner takes many X-ray pictures from different angles around the chest. A computer combines these images to create detailed cross-sectional pictures of the lungs. Radiologists examine these images carefully for any unusual spots or nodules.
LDCT scans can detect lung nodules as small as a few millimeters. Most lung nodules are not cancer, but some may need further testing. The detailed images help doctors see changes in the lungs that might not show up on regular chest X-rays.
Patients do not need to take any special medications or follow dietary restrictions before the scan. Preparing for cancer screening is usually straightforward for lung cancer screening.
Benefits and Limitations of Screening
Research shows that lung cancer screening with LDCT can reduce lung cancer deaths by about 20% in high-risk people. The National Lung Screening Trial found that screening helped detect lung cancer at earlier stages when treatment is more effective.
Early detection of cancer often leads to better treatment outcomes. When lung cancer is found early, before it spreads to other parts of the body, five-year survival rates are much higher than when cancer is found at later stages.
However, screening also has limitations and potential harms. False positive results occur when scans show suspicious areas that turn out not to be cancer. This can lead to anxiety and additional tests that may not be necessary.
Some screening programs detect slow-growing cancers that might never have caused health problems during a person’s lifetime. This is called overdiagnosis. Additionally, repeated CT scans expose people to small amounts of radiation, though the benefits typically outweigh this risk for high-risk individuals.
What to Expect During and After Screening
On the day of screening, patients arrive at the imaging center and check in with staff. They may need to change into a hospital gown and remove jewelry or metal objects that could interfere with the scan. The actual scanning process is quick and painless.
During the scan, patients lie still on their back and may be asked to hold their breath for short periods. The technologist operates the machine from a separate room but can communicate through an intercom. Most people can return to normal activities immediately after the scan.
Results are usually available within a few days to a week. A radiologist reviews the images and sends a report to the ordering healthcare provider. The provider then contacts the patient to discuss results and any next steps that might be needed.
If the scan shows no concerning findings, patients typically continue with annual screening as recommended. If suspicious areas are found, additional testing such as follow-up CT scans, PET scans, or biopsies might be necessary to determine if cancer is present.
Making Decisions About Screening
Deciding whether to have lung cancer screening involves weighing benefits and risks with help from healthcare providers. People should consider their individual risk factors, overall health, and personal preferences when making this decision.
Healthcare providers can help explain screening guidelines and discuss whether someone meets the criteria for screening. They can also address concerns about radiation exposure, false positive results, and what happens if suspicious findings are discovered.
Some people may choose not to have screening even if they meet the guidelines. Others might want screening but fall outside the recommended criteria. Open communication with healthcare providers helps ensure decisions align with individual values and circumstances.
Insurance coverage for lung cancer screening varies, but many plans cover screening for people who meet established guidelines. Patients should check with their insurance providers about coverage details and any out-of-pocket costs.
Beyond Screening: Reducing Lung Cancer Risk
While screening is important for high-risk individuals, preventing lung cancer remains the most effective approach. Quitting smoking is the single most important step people can take to reduce their lung cancer risk, regardless of how long they have smoked.
Studies show that lung cancer risk decreases significantly within years of quitting smoking, though it remains higher than for people who never smoked. Many resources are available to help people quit, including medications, counseling, and support groups.
Other risk reduction strategies include avoiding secondhand smoke, testing homes for radon gas, and minimizing exposure to cancer-causing chemicals at work. Eating a healthy diet rich in fruits and vegetables may also support overall lung health.
Regular physical activity and maintaining a healthy weight contribute to overall wellness and may help reduce cancer risk. People should discuss comprehensive risk reduction strategies with their healthcare providers along with screening recommendations.
Common Myths and Misunderstandings
Myth: Everyone Over 50 Should Get Lung Cancer Screening
Lung cancer screening is recommended only for people who meet specific high-risk criteria, primarily those with significant smoking histories. Most people over 50 do not need lung cancer screening if they have never smoked or have minimal smoking history. Screening guidelines focus on those most likely to benefit from early detection.
Myth: A Normal Screening Result Means You Will Never Get Lung Cancer
Screening can miss some lung cancers, and new cancers can develop between screening appointments. A normal result means no suspicious areas were found at that time, but continued screening and attention to symptoms remain important. People should still see healthcare providers for any concerning respiratory symptoms.
Myth: Lung Cancer Screening Uses Dangerous Amounts of Radiation
Low-dose CT scans use significantly less radiation than regular CT scans while still providing clear images. For high-risk individuals, medical experts agree that the potential benefits of finding lung cancer early outweigh the small radiation risks. The radiation exposure from LDCT is comparable to what people naturally receive from the environment over several months.
Key Takeaways
- Lung cancer screening with low-dose CT scans is recommended for high-risk adults aged 50-80 with significant smoking histories
- Screening can detect lung cancer early when treatment is most effective, potentially reducing lung cancer deaths by about 20%
- The screening process is quick, painless, and requires no special preparation or recovery time
- Benefits include early cancer detection, but risks include false positives, overdiagnosis, and small amounts of radiation exposure
- Healthcare providers help determine if screening is appropriate based on individual risk factors and overall health
- Quitting smoking remains the most important step for reducing lung cancer risk, regardless of screening status
Learn More
- National Cancer Institute Lung Cancer Screening Information – comprehensive guide to screening benefits and risks
- CDC Lung Cancer Screening Guidelines – current recommendations and eligibility criteria
- U.S. Preventive Services Task Force Lung Cancer Screening Recommendation – evidence-based screening guidelines
- World Health Organization Cancer Facts – global perspective on cancer prevention and early detection
- Clinical Trials for Lung Cancer Screening – current research studies on screening methods
- National Cancer Institute Smoking Cessation Information – resources for quitting smoking
- CDC Radon Information – testing and reducing radon exposure to prevent lung cancer
Disclaimer: This information is for educational purposes only and is not medical advice. Talk to a healthcare provider about questions related to your health.