- Current Screening Rates by Cancer Type
- Demographic Patterns in Screening
- Geographic and Access Barriers
- Insurance and Financial Factors
- Cultural and Social Influences
- Healthcare System Factors
- Common Myths and Misunderstandings
- Myth: Only People with Family History Need Screening
- Myth: Screening Always Leads to Unnecessary Procedures
- Myth: Symptoms Always Appear Before Cancer Becomes Serious
- Key Takeaways
- Learn More
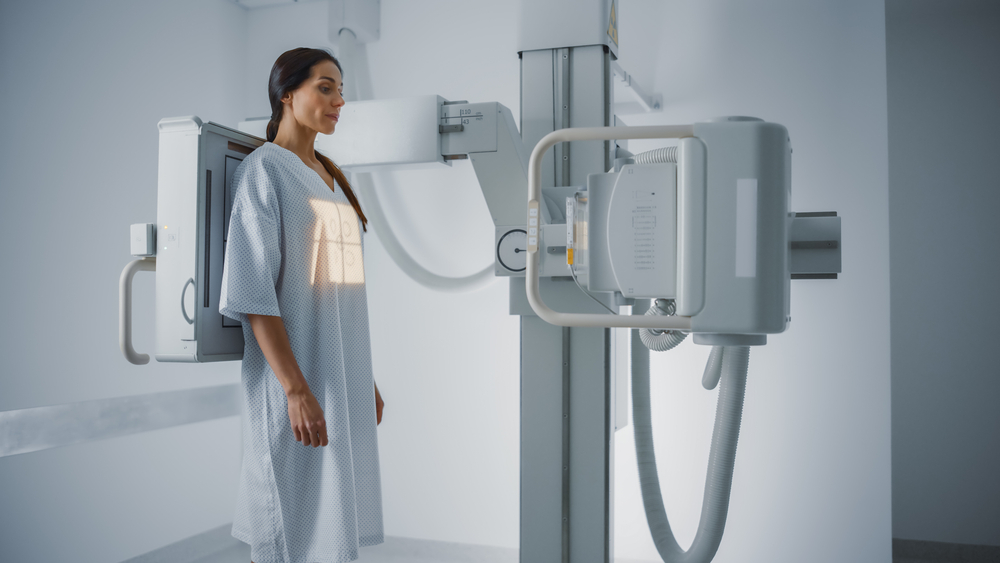
Cancer screening rates vary widely across different groups of people. Some communities have high screening rates, while others face significant barriers. Understanding these patterns helps explain why certain populations experience better cancer outcomes than others.
Multiple factors influence who gets screened and who doesn’t. These include access to healthcare, insurance coverage, cultural beliefs, and geographic location. Research shows these differences contribute to health disparities in cancer detection and survival rates.
Current Screening Rates by Cancer Type
Breast cancer screening has some of the highest participation rates among recommended screenings. Studies show that about 78% of women aged 50-74 have had a mammogram within the past two years. However, rates drop significantly for women without insurance or regular healthcare providers.
Cervical cancer screening rates are also relatively high, with approximately 81% of women aged 21-65 having received appropriate screening. The introduction of HPV testing has improved detection rates, but gaps remain in certain communities.
Colorectal cancer screening lags behind other types, with only about 69% of adults aged 50-75 up to date with recommended screening. This represents significant room for improvement, especially since early detection can dramatically improve outcomes.
Lung cancer screening has the lowest participation rates among major cancer screenings. Despite guidelines recommending screening for high-risk individuals, less than 15% of eligible people receive appropriate screening according to research from the National Cancer Institute.
Demographic Patterns in Screening
Age plays a significant role in screening participation. Adults aged 50-64 typically have higher screening rates than those 65 and older. This pattern reverses the expected trend, since Medicare coverage should improve access for older adults.
Gender differences exist beyond the obvious organ-specific screenings. Women generally participate in preventive health services at higher rates than men. This includes screenings that apply to both genders, such as colorectal cancer screening.
Educational level strongly correlates with screening participation. People with college degrees are significantly more likely to receive recommended screenings compared to those with high school education or less. This pattern holds across all major cancer screening types.
Income levels create substantial gaps in screening access. Higher-income individuals consistently show higher screening rates, even when controlling for insurance status. The Centers for Disease Control and Prevention tracks these disparities through national surveys.
Geographic and Access Barriers
Rural areas face unique challenges in cancer screening access. Limited healthcare facilities, longer travel distances, and fewer specialists contribute to lower screening rates. Some rural counties have no mammography facilities within 50 miles.
Urban areas typically have better access to screening facilities, but disparities exist within cities. Neighborhoods with lower socioeconomic status often have fewer healthcare options and longer wait times for appointments.
Transportation barriers affect many communities. People without reliable transportation may miss screening appointments or avoid scheduling them altogether. Public transportation limitations particularly impact elderly and disabled populations.
Healthcare provider availability influences screening rates significantly. Areas with physician shortages show correspondingly lower screening participation. The shortage of primary care providers particularly impacts preventive services like cancer screening.
Insurance and Financial Factors
Insurance coverage dramatically affects screening participation. Uninsured adults are far less likely to receive recommended cancer screenings. Even among insured populations, differences in coverage types create variations in screening rates.
The Affordable Care Act requirement for preventive services coverage has improved access for many Americans. Most insurance plans now cover recommended cancer screenings without copayments or deductibles. However, gaps remain for people in certain insurance categories.
Underinsurance creates barriers even for people with coverage. High deductibles or copayments can discourage screening participation. Fear of unexpected costs related to follow-up procedures also influences decision-making.
Medicare coverage generally supports screening participation, but confusion about benefits can create barriers. Some older adults avoid screening due to misunderstandings about what Medicare covers or concerns about costs.
Cultural and Social Influences
Cultural beliefs about health and medical care significantly impact screening decisions. Some communities have historical mistrust of medical systems, leading to lower participation in preventive services.
Language barriers affect screening access for many immigrants and non-English speakers. Limited availability of interpreters and translated materials can prevent effective communication about screening benefits and procedures.
Family and social network attitudes influence individual screening decisions. People whose friends and family members participate in screening are more likely to get screened themselves. Community health programs that leverage social connections show promising results.
Religious beliefs sometimes affect screening participation. Some faith communities actively promote preventive health measures, while others may have concerns about certain procedures. Healthcare providers increasingly recognize the importance of culturally sensitive approaches.
Healthcare System Factors
Primary care relationships strongly predict screening participation. People with regular healthcare providers receive recommended screenings at much higher rates. Continuity of care allows providers to track screening schedules and send reminders.
Healthcare system organization affects screening rates. Integrated health systems with electronic health records typically achieve higher screening rates through automated reminders and tracking systems.
Provider communication skills influence patient decisions about screening. Clear explanations about benefits and risks help people make informed choices. Training programs for healthcare providers focus on improving these communication skills.
Appointment scheduling systems can create barriers or facilitate access. Flexible scheduling options, including evening and weekend appointments, improve participation for working adults. Online scheduling systems also increase convenience for many patients.
Common Myths and Misunderstandings
Myth: Only People with Family History Need Screening
Many people believe cancer screening is only necessary if cancer runs in their family. Research shows that most people diagnosed with cancer have no family history of the disease. The U.S. Preventive Services Task Force bases screening recommendations on population-wide risk factors, not just family history.
Myth: Screening Always Leads to Unnecessary Procedures
Some people avoid screening because they fear it will lead to unnecessary tests or treatments. While false positives do occur, the benefits of early detection far outweigh the risks for recommended screenings. Most screening results are normal, and follow-up procedures are only recommended when medically necessary.
Myth: Symptoms Always Appear Before Cancer Becomes Serious
This dangerous misconception leads people to skip screening while feeling healthy. Many cancers develop without obvious symptoms until advanced stages. Screening specifically aims to detect cancer before symptoms appear, when treatment is most effective.
Key Takeaways
- Screening rates vary significantly by cancer type, with breast and cervical cancer having higher participation than colorectal and lung cancer screening
- Demographic factors including age, education, income, and gender create substantial disparities in who receives recommended screenings
- Geographic location affects access, with rural areas facing particular challenges in screening availability and transportation
- Insurance coverage and financial factors remain major barriers, despite improvements from healthcare reform legislation
- Cultural beliefs, language barriers, and social influences significantly impact screening decisions across different communities
- Healthcare system factors like provider relationships and appointment accessibility strongly predict screening participation rates
Learn More
- National Cancer Institute Cancer Screening Overview – Comprehensive information about different cancer screening types and recommendations
- CDC Cancer Screening Data and Statistics – Current data on screening rates across different populations and regions
- U.S. Preventive Services Task Force Cancer Recommendations – Evidence-based guidelines for cancer screening by type and population
- World Health Organization Cancer Facts – Global perspective on cancer prevention and early detection
- ClinicalTrials.gov Cancer Screening Studies – Current research on improving cancer screening methods and access
- How to Prepare for Cancer Screening – Practical guidance for getting ready for different screening procedures
- CDC Colorectal Cancer Screening Information – Detailed information about colorectal screening options and barriers
Disclaimer: This information is for educational purposes only and is not medical advice. Talk to a healthcare provider about questions related to your health.