- What Does Genetic Risk Mean?
- Common Genes Linked to Increased Cancer Risk
- How Genetic Risk Changes Screening Timelines
- Breast and Ovarian Cancer Screening and Genetics
- Colorectal Cancer and Family Genetics
- Why Family History Matters
- Genetic Testing and Screening Decisions
- Emotional and Practical Considerations
- How Genetic Risk Influences Screening Frequency
- Different Screening Tools for People With Genetic Risk
- Genetics and Screening for Multiple Cancer Types
- Screening Recommendations for Children and Young Adults
- How Screening Recommendations Are Personalized
- Genetic Counseling and Screening Guidance
- Balancing Awareness Without Fear
- Talking With Your Healthcare Team About Genetic Screening
- How Genetics Can Help Families Plan Ahead
- What to Remember About Genetics and Screening
- Support and Education Resources
- Conclusion
Cancer screening plays an important role in finding cancer early, when treatment options may be more effective. While many screening guidelines are based on age and general risk factors, genetics can significantly influence when, how often, and which screenings are recommended for certain individuals.
Some people are born with inherited genetic changes that increase their likelihood of developing specific cancers. Understanding how genetics affect cancer risk can help individuals and families make informed decisions about screening and prevention.
This article explains, in clear and simple terms, how genetics influence cancer screening recommendations, who may need earlier or more frequent screening, and why family history matters.
What Does Genetic Risk Mean?
Genetic risk refers to the chance of developing cancer due to inherited changes, also called mutations, in certain genes. These changes are passed down from parents to children and are present from birth.
Not all cancers are genetic. Most cancers develop due to a combination of aging, lifestyle factors, and environmental exposures. However, experts estimate that about 5—10% of cancers are strongly linked to inherited genetic mutations.
Source:
National Cancer Institute — Genetics and Cancer
When someone carries a known cancer-related gene mutation, their lifetime risk for certain cancers may be much higher than average. As a result, healthcare providers may recommend earlier, more frequent, or specialized screening.
Common Genes Linked to Increased Cancer Risk
Researchers have identified several genes that, when altered, are associated with higher cancer risk. Some of the most well-known include:
- BRCA1 and BRCA2 — Linked to breast, ovarian, prostate, and pancreatic cancers
- Lynch syndrome genes (MLH1, MSH2, MSH6, PMS2) — Associated with colorectal, endometrial, ovarian, and other cancers
- TP53 — Related to Li-Fraumeni syndrome, increasing risk for multiple cancer types
- APC — Associated with familial adenomatous polyposis (FAP), which increases colorectal cancer risk
These inherited conditions are uncommon, but when present, they can significantly change screening recommendations.
Source:
Centers for Disease Control and Prevention — Genomics and Cancer
How Genetic Risk Changes Screening Timelines
For people at average risk, cancer screening usually begins at standard ages. For example, colorectal cancer screening may start around age 45, and breast cancer screening commonly begins between ages 40 and 50, depending on guidelines.
However, individuals with inherited genetic risk may be advised to:
- Begin screening at a younger age
- Get screened more frequently
- Use different screening tools than the general population
These changes are designed to detect cancer as early as possible, often before symptoms appear.
Breast and Ovarian Cancer Screening and Genetics
Genetic factors play a major role in breast and ovarian cancer screening decisions.
People with BRCA1 or BRCA2 mutations may have a much higher lifetime risk of breast cancer compared to the general population. Because of this, screening plans may include:
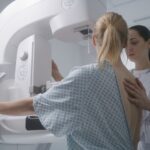
- Earlier mammograms
- Annual breast MRI in addition to mammography
- More frequent clinical breast exams
In some cases, healthcare providers may also discuss additional monitoring strategies, but screening remains a key part of ongoing care.
Source:
American Cancer Society — Genetic Testing for Cancer Risk
Ovarian cancer is more difficult to screen for, but known genetic risk may lead to closer observation and personalized care planning.
Colorectal Cancer and Family Genetics
Colorectal cancer screening is another area where genetics strongly influence recommendations.
Individuals with Lynch syndrome or familial adenomatous polyposis (FAP) often begin colorectal screening much earlier than average-risk individuals. In some cases, screening may start in adolescence or early adulthood.
Screening frequency may also be higher, with exams recommended every one to two years rather than every ten years.
Source:
National Cancer Institute — Genetics of Colorectal Cancer
Why Family History Matters
Even without confirmed genetic testing, family history alone can affect cancer screening recommendations.
Healthcare providers often ask about:
- Cancer diagnoses in close relatives
- Age at diagnosis
- Multiple family members with similar or related cancers
Patterns such as early-onset cancer or several relatives with the same cancer type may suggest inherited risk and lead to earlier or more frequent screening.
Learn more about how cancer risk is evaluated in our related guide:
Understanding Cancer Risk Factors
Genetic Testing and Screening Decisions
Genetic testing can help determine whether a person carries an inherited cancer-related mutation. Test results may influence screening plans, but testing is a personal decision and is not necessary for everyone.
Testing decisions are usually made with the support of trained professionals who explain:
- What the test looks for
- What the results may mean
- How results could affect screening and family members
It is important to understand that genetic testing does not diagnose cancer. It provides information about risk that may help guide future screening choices.
Source:
National Human Genome Research Institute — Genetic Testing
Emotional and Practical Considerations
Learning about genetic cancer risk can bring up many emotions, including concern, uncertainty, or relief. Screening recommendations based on genetics are intended to support early detection and proactive health planning.
Support resources, including genetic counselors and educational organizations, can help individuals better understand screening options and feel more confident in their care decisions.
You may also find helpful guidance in:
Talking to Your Care Team Long-Term
How Genetic Risk Influences Screening Frequency
One of the biggest ways genetics can affect cancer screening is how often screening is recommended. People with inherited cancer risk may be advised to undergo screening more frequently than those at average risk.
More frequent screening is intended to increase the chances of detecting cancer at an early stage, when it may be easier to manage. This does not mean that cancer is expected to occur, but rather that closer monitoring can provide reassurance and early awareness.
For example, individuals with certain inherited colorectal cancer syndromes may be advised to have colon examinations every one to two years instead of every ten years.
Source:
National Cancer Institute — Cancer Screening Overview
Different Screening Tools for People With Genetic Risk
Genetics can also influence which screening tools are recommended. In some cases, standard screening tests may not be enough to provide the most useful information for people at higher genetic risk.
Healthcare providers may recommend additional or alternative screening methods, such as:
- Combining imaging tests instead of relying on a single method
- Using screening tests that can detect changes earlier
- Monitoring multiple organs when a gene is linked to several cancer types
For example, people at higher inherited risk for breast cancer may receive both mammograms and breast MRI scans because each test can detect different types of changes.
Source:
American Cancer Society — Cancer Screening Guidelines

Genetics and Screening for Multiple Cancer Types
Some inherited gene mutations are linked to more than one type of cancer. In these situations, screening plans may include monitoring for several cancers at the same time.
For example, certain genetic syndromes may increase the risk of:
- Colorectal cancer
- Endometrial cancer
- Ovarian cancer
- Stomach or urinary tract cancers
Because of this broader risk, screening recommendations may involve different specialists and a coordinated care plan.
Source:
Centers for Disease Control and Prevention — Hereditary Colorectal Cancer
Screening Recommendations for Children and Young Adults
In rare cases, inherited cancer risk can affect screening recommendations for children or young adults. Some genetic conditions are associated with cancers that may occur earlier in life.
When this happens, screening may begin much earlier than typical guidelines. These decisions are made carefully and are based on established medical consensus and long-term research.
It is important to note that early screening does not mean a child or young adult is expected to develop cancer. Instead, it is a precautionary approach to support early awareness.
How Screening Recommendations Are Personalized
Cancer screening based on genetics is not one-size-fits-all. Screening plans are personalized using several factors, including:
- Specific gene mutation, if known
- Personal medical history
- Family cancer history
- Age and overall health
This personalized approach helps ensure that screening is appropriate, balanced, and aligned with an individual’s specific risk profile.
Learn more about personalized cancer care planning in:
Care Transitions After Treatment
Genetic Counseling and Screening Guidance
Genetic counseling often plays an important role in helping individuals understand how genetics may affect cancer screening. Genetic counselors are trained to explain risk information in clear, understandable terms.
They may help individuals and families:
- Understand genetic test results
- Review family health history
- Discuss appropriate screening options
- Prepare questions for healthcare providers
Genetic counseling supports informed decision-making and helps people feel more confident about their screening plans.
Source:
National Cancer Institute — Genetic Testing Fact Sheet
Balancing Awareness Without Fear
While learning about genetic cancer risk can feel overwhelming, screening recommendations based on genetics are meant to empower individuals–not create fear.
Screening is a proactive step that focuses on awareness and early detection. Many people with inherited genetic risk never develop cancer, and screening helps provide reassurance and peace of mind.
For additional support on managing uncertainty, you may find this resource helpful:
Advocating for Your Health After Cancer
Talking With Your Healthcare Team About Genetic Screening
If you have concerns about genetic cancer risk, open communication with your healthcare team is an important step. You do not need to have all the answers before starting the conversation.
Helpful topics to discuss may include:
- Your personal and family cancer history
- Any known genetic conditions in close relatives
- Questions about when to begin screening
- How often screening may be recommended
Preparing a written list of questions or concerns before appointments can make conversations more productive and less stressful.
You can find additional guidance on long-term communication in:
Talking to Your Care Team Long-Term
How Genetics Can Help Families Plan Ahead
Because inherited genetic changes can affect multiple family members, screening recommendations based on genetics often have implications beyond one individual.
When genetic risk is identified, families may:
- Share health history information with relatives
- Encourage age-appropriate screening
- Support one another in learning about cancer prevention
Family-based awareness can promote earlier detection and informed decision-making across generations.
Source:
National Cancer Institute — Family Cancer Risk
What to Remember About Genetics and Screening
Genetics can influence cancer screening recommendations, but it does not determine outcomes. Screening guidelines are tools designed to support early awareness and proactive care.
Key points to remember include:
- Most cancers are not inherited
- Genetic risk may lead to earlier or more frequent screening
- Family history can affect screening even without genetic testing
- Screening plans are personalized and may change over time
Staying informed and engaged in screening decisions can help individuals and families feel more confident about their health planning.
Support and Education Resources
Reliable education and support resources can help individuals better understand genetic cancer risk and screening options. Learning from trusted, evidence-based organizations can reduce confusion and build confidence.
For additional cancer education and prevention topics, explore related content such as:
Understanding Cancer Risk Factors
Conclusion
Genetics play an important role in shaping cancer screening recommendations for some individuals and families. By understanding inherited risk, people can work with their healthcare teams to create screening plans that support early detection and informed decision-making.
Cancer screening guided by genetic awareness is not about predicting illness–it is about empowering individuals with knowledge and proactive care options.